Medaura Medical Billing is not just another medical billing company. We are an Illinois-based healthcare billing company built for providers who want clarity, compliance, and consistent cash flow. From solo physicians to growing multi-specialty practices, we help healthcare organizations across the USA get paid faster and more accurately.
Billing mistakes, payer delays, and compliance pressure can quietly drain revenue. That is why practices partner with Medaura. We combine hands-on expertise with proven billing workflows to keep your revenue cycle strong and predictable.
Medaura Medical Billing is built for practices that want consistency, visibility, and control over their revenue. Based in Maryland and serving providers nationwide, we manage the whole revenue cycle with precision and accountability.
Certified experts handling Medicare, Medicaid, and commercial billing daily
Complete billing support from coding to claims and credentialing
Proactive AR follow-ups that reduce delays, denials, and unexpected billing gaps
Scalable workflows that grow with your practice
Clear visibility into revenue at every billing stage
Compliance-focused processes that protect against audits
Our end-to-end medical billing services ensure eligibility is confirmed before care is delivered, documentation supports coding accuracy, claims are scrubbed against payer rules, and denials are aggressively appealed.

Medaura provides detailed, easy-to-understand reports covering collections, AR aging, denial trends, and payer performance. These insights help practices spot revenue bottlenecks early and adjust workflows before problems escalate.

Our certified coding team assigns CPT, ICD-10, and HCPCS codes based on provider documentation and current payer guidelines, carefully managing modifiers, bundling rules, and specialty-specific billing nuances to prevent denials or downcoding.

Medaura analyzes each denial to identify its cause, whether from documentation gaps, authorization failures, or payer policy changes. We correct and resubmit claims promptly and prepare detailed appeals with supporting documentation

Eligibility issues remain one of the top causes of claim denials across the U.S. healthcare system. Before services are rendered, we verify patient eligibility, coverage limitations, copays, deductibles, and prior authorization requirements.
Outsourcing medical billing is no longer just about convenience. For many practices, it has become a strategic move to protect revenue, reduce risk, and keep operations running smoothly. When you partner with a professional medical billing company in Illinois like Medaura, the benefits extend far beyond claim submission.


Faster Collections and Healthier Cash Flow

Fewer Denials and Less Revenue Leakage

Reduced Administrative Burden on In-House Staff

Improved Compliance and Lower Audit Risk

Better Visibility Into Financial Performance

Scalability Without Staffing
Headaches
Credentialing errors can stop revenue before the first claim is ever submitted. Medaura manages the full credentialing and enrollment process to ensure providers remain billable without interruption.
We handle Medicare, Medicaid, and commercial payer enrollments; new provider credentialing and re-credentialing; CAQH setup and monitoring; NPI validation; and payer contract coordination. Proper credentialing prevents payment holds, retroactive denials, and costly resubmissions.

Every medical specialty comes with its own billing rules, coding nuances, and payer challenges. At Medaura Medical Billing, we do not force generic billing workflows onto specialized practices. As a seasoned medical billing company in Illinois serving providers nationwide, we tailor our processes to the clinical and financial realities of each specialty.
We understand that what works for a primary care clinic may fail for a specialty practice. Different procedures, documentation standards, modifiers, and reimbursement models require specialty-focused billing expertise. That is precisely what we bring to the table.
Our team works closely with physicians to align coding, claims submission, and payer follow-up with specialty-specific requirements. This approach helps reduce denials, improve reimbursement accuracy, and protect long-term revenue.
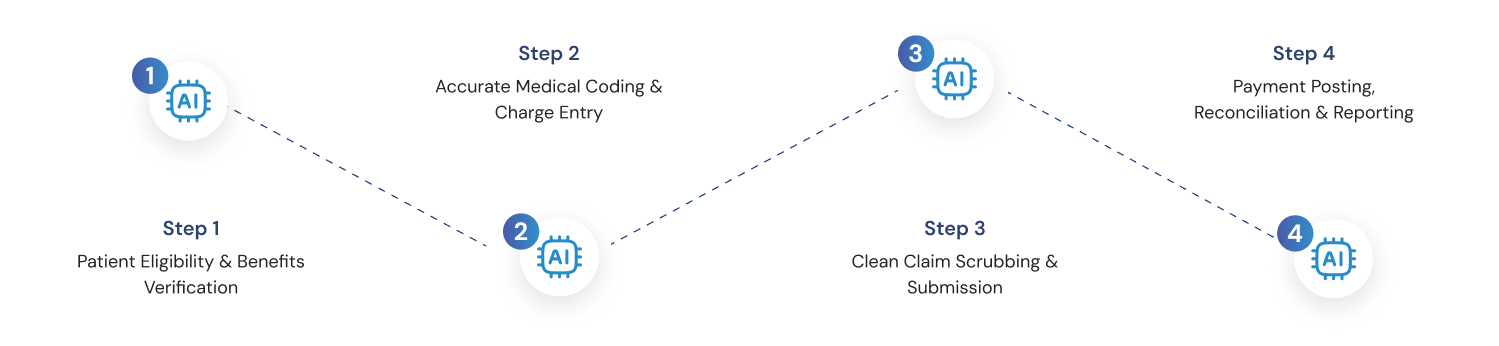
Medaura follows a structured, payer-aligned billing workflow built to reduce denials and accelerate reimbursements.

Medaura Medical Billing works directly within your existing EHR and practice management systems. Our team adapts to your technology instead of forcing costly software changes. This ensures billing stays aligned with clinical documentation and reduces workflow disruptions for your staff.
Medaura offers flexible, practice-friendly pricing models designed to scale with your needs. Whether percentage-based or flat-fee, our pricing remains transparent with no hidden charges or long-term contracts.
All revenue cycle services are included, eliminating per-task billing that inflates costs. Clear monthly invoices and predictable expenses allow practices to budget confidently while achieving measurable ROI.

We provide podiatry billing services across multiple states, ensuring compliance with state-specific payer rules while maintaining consistent billing performance.
We offer expert podiatry billing services in:
Credentialing team has helped me secure out-of-network enrollment with a good insurance company. I trust them completely. has helped me secure

Everything you need in one place: expert RCM insights, a robust medical billing library, and the latest industry updates to keep you ahead.
If you are dealing with frequent denials, delayed payments, growing AR, or staff burnout, outsourcing can be a smart move. A professional medical billing services company brings structure, consistency, and expertise that most in-house teams struggle to maintain. Many practices see measurable improvements within the first few billing cycles.
No. We follow a structured onboarding and transition process designed to avoid interruptions. Our team carefully coordinates data transfer, payer setup, and workflow alignment. Claims continue to move while the transition takes place, ensuring revenue stays on track.
We manage billing for Medicare, state Medicaid programs, and major commercial payers across the USA. Each payer has unique rules and timelines, and our billing experts follow payer-specific guidelines to maximize reimbursement.
We focus on prevention first. Eligibility verification, accurate coding, modifier review, and claim scrubbing reduce errors before submission. When denials occur, our AR team analyzes the root cause and submits timely corrections or appeals to recover revenue.
You receive regular reports covering collections, AR aging, denial trends, and payer performance. We believe transparency is essential, so you always know how your revenue cycle is performing.
We strictly follow HIPAA compliance standards and use secure systems to protect patient information and financial data. Data security and confidentiality are treated as top priorities.
If your practice is struggling with denials, slow payments, or billing stress, now is the time to make a change. Medaura Medical Billing is an Illinois-based medical billing company helping providers across the USA collect more, stay compliant, and regain peace of mind.
We do not believe in quick fixes or cookie-cutter solutions. We take the time to understand your specialty, payer mix, and current billing gaps, then build a long-term billing strategy that works for your practice.
Whether you are outsourcing billing for the first time or switching from another vendor, our transition process is smooth, transparent, and disruption-free.
Let a trusted healthcare billing company handle the complexity while you focus on patient care.
At Meduara Billing, we transform the healthcare revenue cycle with unmatched precision and dedication. As leaders in the medical billing industry, we excel in.