Insurance eligibility verification is where clean billing begins. When coverage details are missed or misunderstood, the result is predictable. Claim rejections rise. Patient satisfaction drops. Cash flow slows. What looks like a small front-office task quickly turns into revenue loss across the billing process.
Medaura Medical Billing is an Illinois-based medical billing company providing insurance eligibility verification services to healthcare providers across the United States.
By confirming eligibility upfront, we help healthcare organizations reduce administrative burdens, submit accurate billing, and protect financial stability across Medicare, Medicaid, and commercial payers.

Eligibility checks are often rushed. Front-office teams juggle phone calls, scheduling, patient check-ins, and data entry simultaneously. In high-volume medical practices, coverage checks become a checkbox instead of a controlled process.
These breakdowns later appear as claim denials and patient disputes.
Common eligibility verification gaps include:
Inactive or recently terminated insurance plans
Incorrect policy numbers, group numbers, or insurance data
Missed prior authorization or referral requirements
Unclear copays, deductibles, and coinsurance amounts
Coverage issues discovered after services are rendered
Our insurance eligibility verification services are designed to support accurate billing and reduce claim denials across all payer types.

We verify patients’ insurance coverage in real time using payer portals and direct insurance checks. Active coverage status, effective dates, and network status are confirmed before the appointment.

Coverage details are reviewed carefully. Copays, deductibles, coinsurance, and coverage limits are confirmed, so patient payment responsibility is clear before services are delivered.

Services that require prior authorization or referrals are identified early. We track approval requirements to prevent claim rejections tied to missing authorizations.

For patients with multiple insurance providers, we verify coordination of benefits. Correct payer sequencing prevents duplicate claims and reduces billing errors.
Insurance eligibility verification is the process of confirming a patient’s insurance coverage, benefits, and payer requirements before medical services are provided. This step validates whether coverage is active, what services are covered, and how costs are shared between the payer and the patient.
Within the healthcare revenue cycle, eligibility verification sits at the very front. When it fails, every step that follows becomes unstable. Claims get rejected. Payments get delayed. Accounts receivable grow. Staff time gets wasted on rework.
Accurate patient eligibility verification supports clean claim submission, improves reimbursement rates, and allows medical practices to make informed decisions before care is delivered. It also sets clear expectations for patient responsibility, which directly improves patient satisfaction.
A structured insurance eligibility verification process protects revenue and reduces claim denials.
Our process includes:
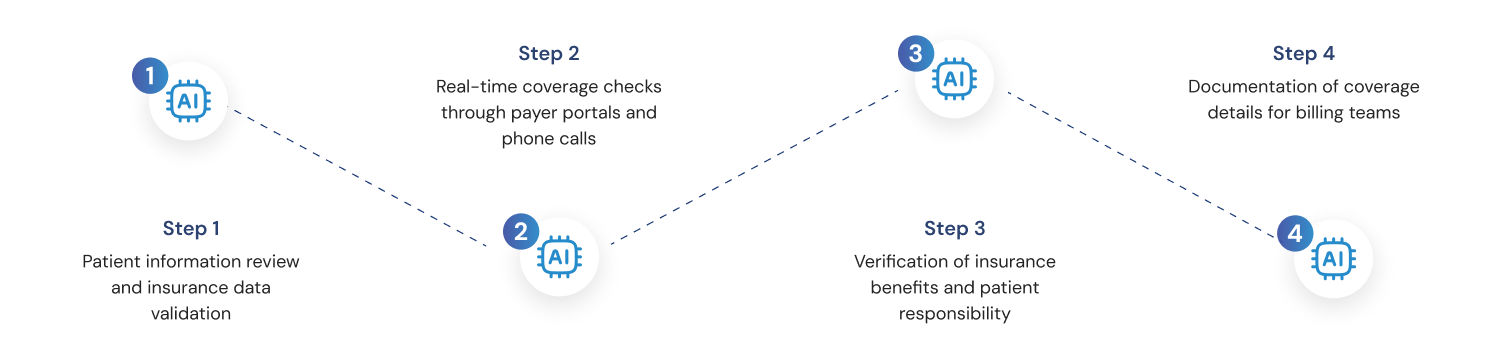
Our team verifies eligibility across a wide range of insurance companies and payer programs.
Medicare and Medicare Advantage plans
State Medicaid and managed Medicaid programs
Commercial insurance providers
Employer-sponsored health plans
Each payer follows different eligibility rules. Our experience across insurance providers ensures compliance and consistency.


While headquartered in Illinois, Medaura provides insurance eligibility verification services across the United States. Our workflows are designed to support multi-location and multi-state medical practices.
We combine strong Illinois payer knowledge with nationwide eligibility verification support. This allows us to deliver consistent coverage checks across locations while adapting to state-specific Medicaid rules and payer requirements.
Our nationwide eligibility verification services support growing practices, health systems, and high-volume clinics with accuracy and scale.
Our services support a wide range of healthcare providers and medical practices.
High-volume clinics with limited staff time
Practices experiencing recurring eligibility-related denials
Healthcare organizations with complex payer mixes
Providers seeking accurate billing and financial stability

Eligibility mistakes lead to denied claims, frustrated patients, and wasted staff time. Practices trust Medaura because we remove guesswork from insurance verification and support accurate billing from the start.
Real-time patient eligibility verification
Clear documentation for billing and audits
Coordination of benefits expertise
Integration with billing and denial management services
Eligibility verification is the first defense against claim denials and revenue loss. When done correctly, it improves cash flow, reduces patient disputes, and stabilizes financial performance.
Outsourcing insurance verification services offers clear advantages:
Fewer claim rejections caused by coverage issues
Reduced administrative burdens on front-office staff
Cleaner insurance claims on first submission
Lower denial rates and faster reimbursements
Improved patient satisfaction through transparency
Eligibility verification confirms a patient’s insurance coverage, benefits, and requirements before services are provided. Accurate verification prevents claim denials, reduces claim rejections, and supports clean billing and timely reimbursement.
Eligibility should be checked 24–72 hours before the appointment and rechecked at the time of service. Coverage details can change, impacting claim submission and patient responsibility.
Yes. Benefits verification services confirm whether specific medical services are covered, whether prior authorization is required, and what out-of-pocket costs apply.
Inaccurate verification leads to coverage issues, claim denials, payment delays, and increased administrative work for billing teams.
Eligibility checks may be handled internally or outsourced to a billing company. The goal is to verify coverage accurately before services to support clean claims and financial stability.
Eligibility verification is not just a front-office task. It is a revenue protection strategy. When coverage checks are accurate, claims move faster, reimbursement rates improve, and patients understand their financial responsibility.
At Meduara Billing, we transform the healthcare revenue cycle with unmatched precision and dedication. As leaders in the medical billing industry, we excel in.